Jun 24, 2020
The trials of life can crush one’s spirit or force one to overcome and create something exceptional out of the rubble. Mary Breckinridge, a 1910 St. Luke’s Hospital School of Nursing alumna, is a fine example of later. Born into a Kentucky family of influence and means, Breckinridge was well educated and well-traveled. She was married in 1904 and widowed by 1906, at age 26. She then completed St. Luke’s nursing program and worked teaching French and hygiene in an Arkansas women’s college. In 1912, she married the president of that school and had two children with him, but her daughter was premature and did not survive; her son died suddenly two years later at age four.
Additional struggles broke the marriage beyond repair and she left her husband in 1918 and worked as a public health nurse while awaiting a posting with the American Red Cross in France. She arrived there after the armistice of WW I and helped to initiate a program to provide food and medical assistance for children, nursing mothers, and pregnant women. While in France, she also spent time in England, observing the conditions of children and mothers there, and became convinced that American women in rural areas would benefit from the help of trained midwives. Ad educational visit to Scotland demonstrated how to provide medical care to a dispersed population.

Returning to the United States, she relocated to Leslie County, Kentucky, which had the highest maternal mortality rate in the country. Here Breckinridge, pictured left, introduced nurse-midwives into the region with the founding of The Frontier Nursing Service in 1925, eventually bringing maternal and neonatal death rates down well below the national average. In 1929, The Frontier Nursing Service staff started the American Association of Nurse-Midwives, a precursor of the American College of Nurse-Midwives, and the first American school of midwifery in New York in 1932. Mary Breckinridge served as director of the FNS until her death on May 16, 1965.
Jun 11, 2020
This is a continuation of a guest blog post by Colleen Stapleton. Colleen is a Patient Navigator with the Liver Education and Action Program (LEAP) at Mount Sinai, where she works to improve linkage to care for patients living with Hepatitis C. You can read the original post here.
Scanning
My first day scanning, the team and I addressed the technology involved in making our Mount Sinai News collection available online. I learned about the scanning specifications to best archive our newsletters digitally. These specifications included 300 dpi (dots per inch), “do not scale,” and others particular to our scanner.
I also learned how to navigate the interesting physical space of the IT office, where the scanner was placed in a small kitchenette. Since I was scanning during lunchtime, I saw a few lunches popped in and out of the microwave. I learned that I could go ahead and put the precious paper newsletters on a non-descript plastic yellow barrel drum object, but under no circumstances should papers be placed on the potentially wet nearby water cooler!
Starting with November of 1958, I began electronically piecing together our carefully preserved collection of Mount Sinai Hospital history.
Folding Paper
Gently unfolding each 60-odd year old newsprint was both a physical challenge and delight. I soon fell into the rhythm of scanning the first page, then the second, then switching to scanning the inserted third and fourth pages. Since the newsletters are not stapled, in total I would carefully reverse the seams of two folded pages, then finish up with the back section of the first folded page.
After a few sessions, I noticed that the newsletters were getting considerably longer – some included 12 pages! This 12-page spread would include a total of three seams, and so unfolding and folding would come to resemble the act of taking apart and putting back together a precious Russian doll.
Troubleshooting
My first day at the scanner I became aware that any file containing more than five pages could not be sent via email to our Archives team account. I made the decision at this time to scan four pages at a time, sending the files to the Archives account in pieces. I soon saw the stacks of newsletters flowing from the “un-scanned” to the “scanned” pile.
After each session I would return to my desk and make sure every issue was represented and the scan quality was good. The various parts of each issue were then virtually ‘stitched’ together. Though some months came and went without Mount Sinai Hospital News editions, each newsletter is marked chronologically with issue numbers.

The first Science News insert of the new Mount Sinai School of Medicine
One of my favorite developments in my scanning came with the advent of the Mount Sinai School of Medicine Science News, an insert that was developed as the medical school was founded and produced more and more significant scientific discoveries. There was also the Mount Sinai Medical Center News title change in November-December 1969 to correspond with the newly built school of medicine. The history of Mount Sinai was expanding before my eyes and I had to ensure my metadata reflected these changes!
Moving Forward with Metadata
After scanning part I of the MSH News archive, the team met with the Aufses Archives’ Digital Archivist to clarify our strategy moving forward. We confirmed our goal of making the Adobe PDFs of the News pages available online, creating a digital index of all MSH News electronic files, as well as providing readers with a search function powered by Optical Character Recognition (OCR) to more easily search the newsletter files.
We identified questions to the tune of “How should we put the PDF files online?” and “how can we most easily create an index to the publication?” We ultimately decided to OCR the PDF documents with Adobe and then dump the words into a database program used by the Aufses Archives called DBTextworks. We started with a few pilot issue files and we identified any necessary metadata fields for our project.
So began an exciting new phase: cleaning and inputting metadata. Unfortunately, this was interrupted by the COVID-19 pandemic and the need to stay home, and we have not been able to continue the scanning. However, the work continues with the efforts of a fantastic new summer intern working remotely — soon all of the scanned issues will be described and searchable.
Stay tuned for more blog installments exploring this digitization project along with coverage of the many unique historical Sinai snapshots found in the MSH News!
Jun 4, 2020
An update to this blog post can be found here.
Founded in 1892, the early history of Mount Sinai Beth Israel Hospital was decorated with a series of success stories in the treatment of disease. Against the background of Manhattan’s Lower East Side, then affected by poverty, close living quarters, and dangerous working conditions, its residents, largely recent Jewish immigrants, were made vulnerable to many of the contagious diseases of that era. In its first years, Beth Israel contributed research to combat the typhoid epidemic of 1906-1907, established an after-care clinic to children affected by the 1916 polio epidemic, and is credited with finding the cure for trachoma, which had previously been a cause to turn away new immigrants at Ellis Island.
Only twenty-five years after Beth Israel’s opening, the United States was embroiled in the first World War. The Hospital encouraged its medical staff to join the Medical Reserve Corps, with approximately half of its doctors signing up. The Hospital had also encouraged its nurses, physicians and other staff to join the war effort.
This left Beth Israel in a precarious position when the 1918 Influenza epidemic reached New York City. Being chronically understaffed, Beth Israel’s Medical Board contacted the Department of Health for advice. The response was simply: “There is nothing to advise except the use of gauze masks which did not always prevent the disease.” In November 1918, the Hospital eliminated visiting hours, curtailed teaching hours, and turned the Male Medical Ward over to the Department of Health to use as an isolation facility for the pandemic. (The DOH never used the facility because they were similarly understaffed.)
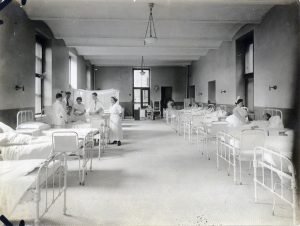
Female ward of Beth Israel Hospital, Jefferson and Cherry Street, circa 1910
Ultimately, Beth Israel was only able to admit twenty-nine influenza patients. (Update: This number is disputed in other sources.) Seven members of the House Staff were awarded $25 (approximately $500 today) for “self-sacrificing services performed” and the Hospital offered special incentive pay to doctors and nurses to help combat the fact that they were understaffed.
Despite the limited patient intake, Beth Israel’s contributions to the 1918 flu pandemic were still impactful. In December 1918, Superintendent of the Hospital, Louis J. Frank, contacted Presidents Roosevelt and Taft to encourage universal nursing training in the education of women, likely in response to the chronic under-staffing at this time. By January 1919, many of the patients in the Hospital were admitted for “post-influenzal complications” leading to the care of many affected by the pandemic.
Sources:
Authored by Stefana Breitwieser, Digital Archivist



