Nov 24, 2020
Whenever you look back to the past, it is easy to find it all very strange, but a longer look allows us to see the threads that connect that time to this. Some of those threads are strong and enduring and others fray and end.
One of those strong threads that tie the Mount Sinai of 100 years ago to the Mount Sinai of 2020 is research and discovery. In 1920, Mount Sinai was dealing with the last wave of a deadly worldwide pandemic that had started in 1918 but still lingered. Some Mount Sinai physicians spent a great deal of time working on a “peculiar disease” that followed the epidemic. This was popularly called the ‘sleeping sickness,’ but doctors termed it epidemic encephalitis. Another Mount Sinai physician was lending his expertise as a member of a national commission that was established to deal with the ravages of empyema, which too often followed post-influenzal pneumonia. Other physicians were doing research on gastric diseases, leukemia, surgical innovations and cardiac problems – all topics that Sinai doctors continue to pursue.

Taken from 5th Ave. and 99th St. looking east over the new buildings. The building facing with the flag pole is the 1904 main building.
Another main theme from 100 years ago, as in every decade of Mount Sinai’s existence, was the physical changes being made on campus. The world war and epidemic had delayed the progress of the largest expansion plan ever envisioned by The Mount Sinai Hospital. First suggested in 1913, it was only in 1922 that all of the new buildings were completed and the renovations of older spaces finished. This resulted in a new Private Pavilion (our current Kravis Children’s Hospital), a new pediatric pavilion and pediatric clinic building, a larger employee dormitory, a larger laboratory building, and a new auditorium to accommodate Mount Sinai’s increasing educational efforts. The growth in the number of beds called for a larger house staff than before and allowed for the growth of new specialty services.
W hile these themes have echoes with our current year, as does the perennial nursing shortage of that era (among many others), there was much that was unique to Mount Sinai in 1920. In February of that year, Mount Sinai leaders held an event to celebrate the staff that had served in the World War I Mount Sinai affiliated unit, Base Hospital No. 3. Special commemorative medals were given to each veteran.
hile these themes have echoes with our current year, as does the perennial nursing shortage of that era (among many others), there was much that was unique to Mount Sinai in 1920. In February of that year, Mount Sinai leaders held an event to celebrate the staff that had served in the World War I Mount Sinai affiliated unit, Base Hospital No. 3. Special commemorative medals were given to each veteran.
The other topic of great interest in 1920 was the re-structuring of the medical staff to combine the in-patient and out-patient services under the in-patient chief of service. The Dispensary and the ward service had been two separate entities with limited overlap. The change allowed the clinic physicians to follow their patients when admitted to the hospital wards, and the ability to round and work with the in-patient staff made it more appealing to community physicians to take on clinic work. In the 1920 Annual Report, it was noted that the combined medical staff now numbered 250 physicians.
Certainly, times change. Institutions changes. Medicine changes. But even 100 years later, at Mount Sinai, some things never change.
Nov 9, 2020
I recently read a piece about Hamilton Square in the Roosevelt Island Historical Society’s From the Archives email. This park, which was named for Alexander Hamilton, existed on the Upper East Side of Manhattan from around 1807-1869. I found this fascinating since The Mount Sinai Hospital moved to Lexington Ave. and 66th St. in 1872. I knew that the City had ‘seeded’ this area with non-profit entities: Hunter College, many hospitals and schools, but I had never heard about the Square itself, which ran from 66th to 69th Streets between 3rd and 5th Avenues. Finally, Mount Sinai had a Hamilton connection, even though he died in 1804, 48 years before the Hospital was created!
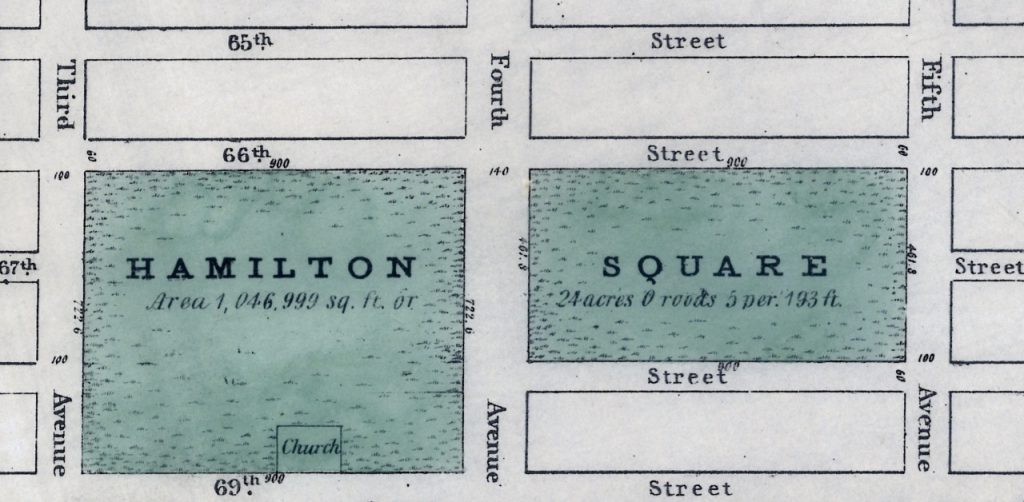
Map of Hamilton Square from the New-York Historical Society
When the Square was broken up, The Mount Sinai Hospital (MSH) was located on W. 28th Street, between 7th & 8th Avenues. It had been founded in 1852 as the Jews’ Hospital in the City of New York (the name was changed in 1866) and had opened its first building in 1855. After the Civil War, the leadership realized that the facility was inadequate and the location less than ideal due to the growth of the City. On November 2, 1867 the Directors authorized the purchase of ten lots of land from 65th to 66th Street on the west side of Park (then 4th) Ave. and later added eight more lots there. But then on October 6, 1868, the City leased Mount Sinai twelve lots of land between 66th and 67th on Lexington Ave. for $1 a year for 99 years. Somehow, over the interim, the City and Mount Sinai had reached an agreement on the Hospital taking over part of the former Hamilton Square. The earlier lots were later sold, saving Mount Sinai thousands of dollars. On May 25, 1870, the cornerstone for the second MSH was laid. The President of the Hospital, Benjamin Nathan, and Mayor Oakley Hall were there. (Within two months, Nathan was murdered in his bed on a ‘dark and stormy night.’)

On May 29, 1872, a dedication ceremony was held for the new Mount Sinai Hospital. When the building opened, it had a greatly expanded capacity of 110 beds. The building was designed by the well-known architect, Griffeth Thomas, and cost $335,000 to complete. It had an operating room in the basement of the north wards, rooms for our newly created House Staff to live in, a meeting room for the Directors, and a synagogue. Lexington Ave. remained unpaved for two more years, and the Hospital never wired the facility for electricity. A telephone was installed in 1882; the number was “Thirty-Ninth St., 257”. It was at this site that Mount Sinai transformed into what we would recognize as a modern hospital, with medical education and research joining its core mission of providing patient care.
In typical Mount Sinai fashion, this facility quickly became too small. Additional buildings were built and major renovations were begun in 1882. In 1890, Mount Sinai added a building across from the Hospital on the north side of 67th St. for our nursing school and Out Patient Department. This building is the only remnant of Mount Sinai that remains there today. It later served as the home of the Neurological Institute, the Polish legation, and finally became a school for the Archdiocese of NY. The Mount Sinai Hospital moved from Lexington Ave. in 1904 to its current East Side location on 100th St., between Madison and 5th Avenues. The name of Hamilton continues on various buildings and neighborhoods of the City, making its most recent appearance on Broadway.
Oct 16, 2020
Our web archives are available online here.
In March 2020, the world began witnessing history in real-time, and archivists scrambled to ensure that the story of COVID-19 would be well-preserved. But with so much happening at a distance, much of the communication and ephemera created in the last six months is online, meaning that archivists have had to eschew traditional practices in collecting physical material and focus increasingly on the enormous amount of material now online. For example, at the peak of the crisis, healthcare institutions like Mount Sinai were updating their websites multiple times a day so that staff and the public had the best and most recent information on policies and procedures regarding things like new treatments and personal protective equipment. This type of information will be valuable moving forward as historians try to understand a rapidly evolving crisis.
Fortunately, technology exists to capture every version of these websites as they appear online. Web archiving has been a practice since the late-1990s, and since 2015 the Aufses Archives has used Archive-It, a web archiving service provided by the Internet Archive, to regularly capture information related to the Mount Sinai Health System. We also use this tool to capture web content related to the response to COVID-19, as well as day-to-day changes to the website.
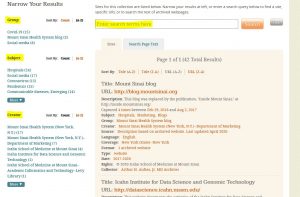
Screenshot of the Aufses Archives page on Archive-It.
The easiest way to access our web archives is to browse the list of websites on the main screen. These results can be filtered using the groups, subjects, or creators on the left side of the screen. You can also use the search bar at the top of the screen to search the metadata created by the archivist. (We expect our COVID-19 group to be the most used group for the foreseeable future.) Information on COVID-19, as well as a wide range of subjects, has been collected by a number other academic institutions, and you can also browse their collections here.
If you’re searching for a particular webpage instead of a whole website, or if you’re trying to search the original text of a website, the “Search Page Text” option may be of use. This feature supports keyword searching of individual web pages, much like Google. However, you can also filter by “Capture date range” which means you can search not just across subjects, but also across time.
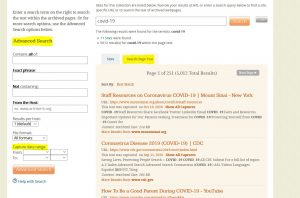
Screenshot of the “Search Page Text” functionality in Archive-It, after searching “COVID-19.”
With either searching method, once you’ve selected a link, you’ll be taken to a page of dates, each corresponding to a particular date of capture. While there’s no guarantee that every version of the website was captured, it will at least give you a sense of how the site has progressed over time.

This page, related to the COVID-19 pandemic, had 72 captures at the time of writing, starting every day from March 23, 2020, to May 12, 2020. The crawl now occurs monthly, due to fewer updates of the website.
Once you’ve selected a date, you’re taken to a version of the website captured on that date. Shown below is our earliest Archive-It capture of the Mount Sinai Hospital homepage, as it appeared in February 2015. The website should play back in the same was as it originally appeared.
Of course, the Mount Sinai Health System only represents a very small corner of the internet, and archivists are working to capture as much as possible. All the websites captured by the Aufses Archives contribute directly to the Internet Archives’ Wayback Machine, which at the time of writing has 477 billion website captures, including a limited number of Mount Sinai webpages dating back to the 1990s, captured on an ad hoc basis. You can also contribute by adding URLs via the link on the Wayback homepage.
Authored by Stefana Breitwieser, Digital Archivist
Aug 27, 2020
This is a guest blog post by summer intern, Lily Stowe-Alekman. Lily is a junior at Smith College where she studies History, Archives, and the Study of Women and Gender.
Even before given access to traditional pathways of change, women at The Mount Sinai Hospital have worked to make change in the institution. From the opening of The Mount Sinai Hospital in 1855, the wives and daughters of the Board of Trustees worked to provide services in order to provide comfort to patients and to address their social and emotional well-being. By 1917, the first year that women were allowed on the Board, the role of women, and their expectations of that role, had substantially changed. The growing power of women was expressed by the creation of their own organization to exert influence over the life of the Hospital, the Social Service Auxiliary. And according to Helen Rehr, DSW, the second Edith J. Baerwald Professor of Community Medicine (Social Work), they were a force to be reckoned with.1 When prompted in an interview about the Auxiliary, “…they weren’t social butterflies having their tea. That’s not an image you would draw,” Rehr responded “Not these women, never. In the 28 years that I’ve known them I don’t recall having tea with them. No, they were women who came with a commitment to the social organization.” Hortense Hirsch, who served on the Auxiliary Board and Board of Trustees as one of the first woman able to be a Trustee, is a powerful example of the trailblazing women of the Auxiliary Board.

A portrait of Hortense Hirsch, circa 1960.
In 1923, Mrs. Hortense Hirsch (1887-1990) began her work with the Social Services Auxiliary (today’s Auxiliary Board), of which she would continue to be a member for sixty-five years, including a tenure as president from 1951-1956. From there, she was elected to the Board of Trustees in 1932, where she remained until becoming an honorary trustee in 1986. She sat on several committees of the Board, including as a member of the Committee on Building Maintenance and Equipment, Vice-Chairman of the Committee on Social Service, Chairman of the Committee on Convalescent Care, and as a member of the Committee on Ladies’ Auxiliary. Hirsch was president of the Neustadter Home for Convalescents beginning in 1937 when the Home affiliated with Mount Sinai, until she stepped down from the post in 1953.

A photograph of (from left to right) Helen Benjamin, member of the Women’s Auxiliary Board; Mrs. Edith Lehman, the first President of the Auxiliary Board from 1916-1917, Mrs. Ruth Cook, President from 1917-51; and Mrs. Hortense Hirsch, the presiding President of the Board at the fiftieth anniversary of the Auxiliary Board in 1956. Helen Benjamin holds a picture of the first social work volunteer from 1907.
Hortense Hirsch lived to be 103 years old, and by all accounts she remained steadfast in her dedication to social work and volunteerism for her whole life. After she graduated from Smith College in 1907 at the age of 19, she married Walter Hirsch and then moved to New York City in 1909. She began her work as a volunteer at Mount Sinai in 1917. The Federation of Jewish Philanthropies later referred to her as the “honorary ‘Dean of Social Work Volunteers.’” As a thoroughly involved volunteer and then Auxiliary Board member, Hirsch dedicated many hours to the hospital. Dr. Helen Rehr remarked in 1982, “The demands on her were great, but she always rose to it. There was no question on that score.”

Portrait of Hortense Hirsch, circa 1976.
Hortense Hirsch’s personality leaps off the pages of archival materials. When at Smith College, she maintained her own horse and buggy, which was against the rules, by paying a farmer for boarding, effectively evading the administration. In a New York Times article documenting her 100th birthday celebration, her daughter Carol Kridel told them, that while Hirsch was too ill to attend and she had to stay in bed, she was still “wearing a pink bedjacket and a pink bow in her silver hair.” The article also includes a story of Hirsch “[coming] to her 85th birthday and [tossing] her skirts high to show she approved of the latest rage—hotpants.”
Hortense Hirsch’s work on the Social Service and Women’s Auxiliary Board helped to transform the hospital. She worked tirelessly as a volunteer and board member. Hirsch’s work and legacy came from and continued those of the women who originally found pathways to affect changes at The Mount Sinai Hospital in the late 1800s. Hirsch served on the Board of Trustees, an opportunity that was not available to the women of previous generations. As Dr. Helen Rehr stated, “the Mrs. Hirsches are an outgrowth of that group of women who were the wives of the board of trustees” and ultimately transformed the hospital in the process.
Aug 21, 2020
This is a guest blog post by summer intern, Lily Stowe-Alekman. Lily is a junior at Smith College where she studies History, Archives, and the Study of Women and Gender.
As a summer intern with the Arthur H. Aufses, Jr., MD Archives, I have become acquainted with Mount Sinai’s history and the efforts that go into preserving its legacy. One of the projects I have worked on is cataloging The Mount Sinai Hospital News, an in-house tabloid-style newsletter for Mount Sinai employees. Colleen Stapleton, Patient Navigator for the Liver Education & Action Program at Mount Sinai, volunteered with the Archives this spring and digitized the newsletters from 1958-71. In my work cataloging, I read some really entertaining stories that offered a glimpse into the personal lives of people who worked in The Mount Sinai Hospital (later Medical Center), whether that be birth announcements of their children, quirky stories about the things employees did outside of the hospital, or articles about celebratory dinners and ceremonies. One can also not forget the hospital’s bowling team.
While cataloging in July, I came across a story that made me pause because it felt like a full circle moment. The October 1971 issue of The Mount Sinai Medical Center News featured an article called “Everyone Talks about Mount Sinai’s Glorious History; Dr. Al Lyons, Arch Archivist, Does Something About It.” This article has history of the Aufses Archives and is within the archive. While the Aufses Archives is a site of historical preservation, it has its own history as well.

Caption: The objects featured in the article header are still in the Arthur H. Aufses Jr. MD Archives today!
The creation of what is now the Arthur H. Aufses, Jr., MD Archives is due to the work and advocacy of Dr. Albert S. Lyons in the 1960s to 1980s. Over this time, Dr. Lyons advocated for the need of creating the archive and in 1986, secured its future with the hiring of a full-time archivist, Barbara Niss, who remains the Director today. Dr. Lyons (1912-2006) spent over sixty years of his life working at Mount Sinai. He began as a surgical resident at Mount Sinai Hospital in 1938. He went on to become the founder and Chief of the Intestinal Rehabilitation Clinic and worked to help support patient needs post-surgery. He was also a Clinical Professor of Surgery at the Mount Sinai School of Medicine. He wrote a well-known book, Medicine: An Illustrated History, a volume of over six hundred pages, charting medicine from the prehistoric era to the twentieth century.
Beyond his clinical work, Dr. Lyons was committed to Mount Sinai’s institutional history and to history of medicine in general. He taught the History of Medicine elective courses in the medical school. In the 1960s, he convinced the hospital board to collect the institutional history of the hospital. In 1966, he was made Hospital Archivist by Mr. Gustave L. Levy, the Chairman of the Board of Trustees. Dr. Lyons’ passion for preserving the history of The Mount Sinai Hospital overlapped with the discussions and planning of Mount Sinai School of Medicine, which welcomed its first students in the fall of 1968. In 1970, he was given the official title of Medical Center Archivist. Dr. Lyons also contributed a broad range of valuable materials to the Archives, including over eighty-five oral history interviews dating to 1965, a formative time for the field of oral history as well as for the Medical Center, as the School planned for and welcomed its first students.
In October of 1971, The Mount Sinai Medical Center News wrote about Dr. Lyons’ archival work. The article highlights the work and efforts of Dr. Lyons and serves as a call to action of sorts for the archive. Dr. Lyons is quoted in the first line as saying, “When in doubt, don’t throw it out.” He goes on to say that “too much of Mount Sinai’s past has already gone up in smoke,” due to people throwing out items without realizing their significance. He stresses as well that ordinary everyday materials are archival. He stresses that history is not necessarily in the distant past, that the events of the previous day are history. In this sense, Dr. Lyons de-mystifies the archives by showing that it should be in connection with the present moment and is not a disconnected abstract institution. The closing paragraph of the article instructs readers, “If you’ve uncovered some papers or objects you think may be worth saving, are planning some event to make current Medical History, etc. Drop Dr. Lyons a note.” In turn, “He and the Future will thank you!”
SOURCES
Arthur H. Aufses, Jr. MD Archives and Records Management. “Lyons, Albert S., MD, Papers, 1932-2000.” Collection Guides. https://icahn.mssm.edu/about/ait/archives/collection/albert-lyons.
Aufses, Arthur H., Jr., and Barbara Niss. This House of Noble Deeds: The Mount Sinai Hospital, 1852-2002, New York University Press, 2002. ProQuest Ebook Central, xi.
“Everyone Talks About Mount Sinai’s Glorious History; Dr. Al Lyons, Arch Archivist, Does Something About It.” Mount Sinai Medical Center News. October 1971. 5, 10.

 hile these themes have echoes with our current year, as does the perennial nursing shortage of that era (among many others), there was much that was unique to Mount Sinai in 1920. In February of that year, Mount Sinai leaders held an event to celebrate the staff that had served in the World War I Mount Sinai affiliated unit, Base Hospital No. 3. Special commemorative medals were given to each veteran.
hile these themes have echoes with our current year, as does the perennial nursing shortage of that era (among many others), there was much that was unique to Mount Sinai in 1920. In February of that year, Mount Sinai leaders held an event to celebrate the staff that had served in the World War I Mount Sinai affiliated unit, Base Hospital No. 3. Special commemorative medals were given to each veteran.









